Health Insurance Claim Process: A Complete Step-by-Step Guide
Health insurance is designed to reduce the financial burden of medical expenses. However, many people are unsure about how to actually use their insurance when medical treatment is required. This is where understanding the health insurance claim process becomes important.
The health insurance claim process is the procedure through which a policyholder requests payment or reimbursement from an insurance provider for medical expenses. It allows individuals to recover healthcare costs that are covered under their policy. Whether the treatment involves a routine hospital visit, surgery, or emergency care, submitting a claim ensures that the insurer pays its share of the cost.
For many people, the claims process can seem confusing. It often involves documents, hospital records, policy verification, and approval procedures. Without proper knowledge, mistakes during the claim process can lead to delays or claim rejection.
Understanding how the system works can help policyholders prepare the right documents, follow the correct steps, and avoid unnecessary complications. This guide explains the health insurance claim process in simple terms, including types of claims, steps involved, documentation requirements, common mistakes, and practical examples.
By learning the claim process clearly, individuals can use their health insurance benefits more effectively and manage medical expenses with greater confidence.
Health Insurance Claim Process Overview
| Step | Description | Who Handles It | Purpose |
|---|---|---|---|
| Medical Treatment | Patient receives healthcare services | Patient and hospital | Start of claim process |
| Claim Notification | Insurer is informed about treatment | Policyholder or hospital | Begins claim request |
| Document Submission | Bills and medical records are submitted | Policyholder or hospital | Provides proof of treatment |
| Claim Verification | Insurer reviews documents and policy details | Insurance company | Confirms eligibility |
| Claim Approval or Rejection | Decision made on the claim | Insurance company | Determines payment |
| Payment or Reimbursement | Approved funds are paid | Insurer | Completes claim process |
, benefits, and financial protection options available to policyholders. Many readers compare multiple guides before selecting a plan so they can clearly evaluate premiums, claim procedures, and long‑term advantages. A useful resource to explore is Insurance Tips for Beginners, which explains how this insurance policy works, the key benefits it offers, and situations where it may be the most suitable option. By reviewing this guide, you can gain deeper insights into coverage features, eligibility requirements, and practical tips that help individuals and families make smarter insurance decisions.
What Is the Health Insurance Claim Process?
The health insurance claim process is the formal procedure through which a policyholder requests payment from an insurance company for medical expenses covered under their health insurance policy.
The process usually involves several steps, including:
-
Notifying the insurance company
-
Submitting medical documents
-
Verification by the insurer
-
Claim approval or rejection
-
Payment or reimbursement
Claims help ensure that the policyholder receives financial assistance according to the terms of their insurance policy.
Types of Health Insurance Claims
Health insurance claims generally fall into two main categories.
Cashless Claims
Cashless claims occur when the insurance company pays the hospital directly for medical services.
Key Characteristics
-
Patient receives treatment at a network hospital
-
Insurance company settles the bill directly
-
Policyholder may only pay non-covered expenses
How It Works
-
Patient visits a network hospital.
-
Hospital contacts the insurance provider.
-
Pre-authorization is obtained.
-
Treatment is provided.
-
Insurance company pays eligible costs directly.
Advantages
-
Less financial burden during treatment
-
Minimal paperwork for the patient
Reimbursement Claims
Reimbursement claims occur when the patient pays medical bills first and later requests reimbursement from the insurance company.
Key Characteristics
-
Used for treatment at non-network hospitals
-
Patient pays hospital bills upfront
-
Insurance company reimburses eligible costs after claim approval
How It Works
-
Patient receives treatment.
-
Patient pays hospital bill.
-
Claim documents are submitted.
-
Insurance company reviews documents.
-
Approved amount is reimbursed.
, benefits, and financial protection options available to policyholders. Many readers compare multiple guides before selecting a plan so they can clearly evaluate premiums, claim procedures, and long‑term advantages. A useful resource to explore is Cheapest Car Insurance in Texas, which explains how this insurance policy works, the key benefits it offers, and situations where it may be the most suitable option. By reviewing this guide, you can gain deeper insights into coverage features, eligibility requirements, and practical tips that help individuals and families make smarter insurance decisions.
Key Terms in the Health Insurance Claim Process
Understanding these terms makes the claims process easier to navigate.
Claim Form
A claim form is the official document used to request reimbursement or payment from the insurer.
It usually includes:
-
Patient information
-
Policy details
-
Hospital information
-
Treatment description
Pre-Authorization
Pre-authorization is approval from the insurer before certain treatments are performed.
This is commonly required for:
-
Surgeries
-
Hospital admissions
-
Specialized treatments
Network Hospitals
Network hospitals are healthcare providers that have agreements with insurance companies.
Benefits include:
-
Cashless treatment options
-
Faster claim processing
Claim Settlement
Claim settlement refers to the final decision made by the insurance company regarding payment.
The insurer may:
-
Approve the full claim
-
Approve partial payment
-
Reject the claim
Claim Processing Time
Claim processing time is the period required by the insurance company to review and settle a claim.
This timeframe may vary depending on:
-
Policy terms
-
Document completeness
-
Claim complexity
Step-by-Step Health Insurance Claim Process
Understanding the step-by-step procedure can help avoid confusion.
Step 1: Receive Medical Treatment
The claim process begins when the insured individual receives medical treatment.
This could include:
-
Hospitalization
-
Emergency treatment
-
Diagnostic procedures
-
Surgery
Step 2: Notify the Insurance Company
Policyholders or hospitals should inform the insurance company as soon as possible.
Notification may include:
-
Policy number
-
Patient details
-
Hospital admission information
Early notification helps avoid claim delays.
Step 3: Submit Required Documents
The next step involves submitting medical and billing documents.
Common documents include:
-
Hospital bills
-
Medical reports
-
Discharge summary
-
Prescription records
-
Claim form
Complete documentation is essential for claim approval.
Step 4: Claim Verification
The insurance company reviews the submitted documents.
Verification may include:
-
Checking policy coverage
-
Confirming treatment details
-
Verifying hospital records
This stage ensures that the claim follows policy rules.
Step 5: Claim Decision
After verification, the insurer makes a decision.
Possible outcomes include:
-
Full approval
-
Partial approval
-
Claim rejection
If additional information is required, the insurer may request more documents.
Step 6: Payment or Reimbursement
If the claim is approved:
-
The insurer pays the hospital (cashless claim), or
-
The insurer reimburses the policyholder.
This step completes the claim process.
, benefits, and financial protection options available to policyholders. Many readers compare multiple guides before selecting a plan so they can clearly evaluate premiums, claim procedures, and long‑term advantages. A useful resource to explore is Insurance Claim Delay Reasons, which explains how this insurance policy works, the key benefits it offers, and situations where it may be the most suitable option. By reviewing this guide, you can gain deeper insights into coverage features, eligibility requirements, and practical tips that help individuals and families make smarter insurance decisions.
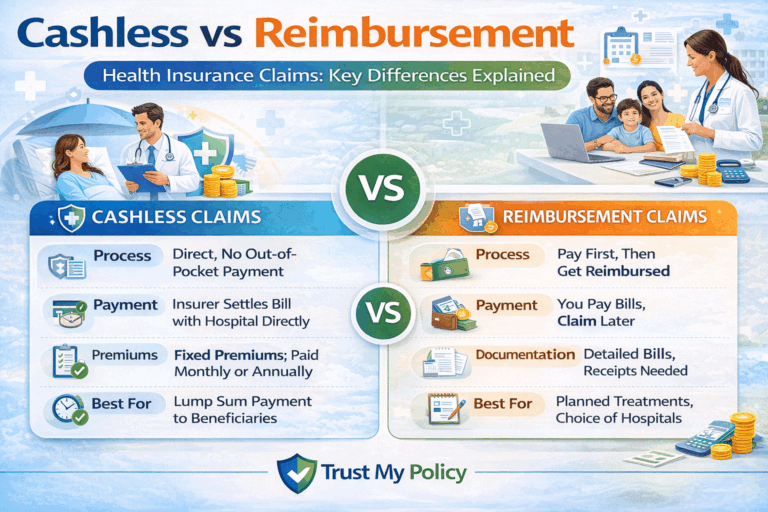
Detailed Comparison: Cashless vs Reimbursement Claims
| Feature | Cashless Claim | Reimbursement Claim |
|---|---|---|
| Payment Method | Insurance company pays hospital directly | Patient pays first and claims reimbursement |
| Hospital Requirement | Network hospital | Any hospital |
| Upfront Payment | Minimal or none | Full payment required |
| Documentation | Mostly handled by hospital | Patient submits documents |
| Processing Time | Often faster | May take longer |
| Convenience | Higher convenience | More paperwork |
Pros and Cons of the Health Insurance Claim Process
Pros
Financial Support
Claims help reduce the cost of medical treatments.
Access to Medical Care
Insurance claims allow patients to receive necessary healthcare without full financial burden.
Cashless Treatment
Network hospitals can provide treatment without requiring immediate payment.
Policy Benefits Utilization
Claims allow policyholders to use the coverage they have purchased.
Cons
Documentation Requirements
The process may require multiple documents and forms.
Processing Time
Claims can take time depending on verification procedures.
Possible Claim Rejection
Incomplete documentation or policy exclusions may lead to rejection.
Policy Limitations
Insurance policies may not cover every medical treatment.
Real-Life Examples of Health Insurance Claims
Example 1: Emergency Hospitalization
A patient is admitted to a network hospital due to an emergency.
Process:
-
Hospital contacts insurer
-
Pre-authorization is approved
-
Treatment is provided
-
Insurance company settles most of the hospital bill
Example 2: Treatment at a Non-Network Hospital
A traveler receives treatment at a hospital not connected to the insurance network.
Process:
-
Patient pays hospital bill
-
Submits claim documents later
-
Insurance company reimburses eligible amount
Example 3: Planned Surgery
A patient schedules surgery in advance.
Process:
-
Hospital requests pre-authorization
-
Insurer approves treatment
-
Surgery performed
-
Claim settled directly
, benefits, and financial protection options available to policyholders. Many readers compare multiple guides before selecting a plan so they can clearly evaluate premiums, claim procedures, and long‑term advantages. A useful resource to explore is Can You Have Multiple Life Insurance Policies, which explains how this insurance policy works, the key benefits it offers, and situations where it may be the most suitable option. By reviewing this guide, you can gain deeper insights into coverage features, eligibility requirements, and practical tips that help individuals and families make smarter insurance decisions.
Common Mistakes in the Health Insurance Claim Process
Many claim issues occur due to simple mistakes.
Delayed Claim Notification
Not informing the insurance company promptly can cause claim complications.
Missing Documents
Incomplete paperwork may delay claim processing or cause rejection.
Ignoring Policy Terms
Some treatments may not be covered under certain policies.
Not Using Network Hospitals
Choosing a non-network hospital may require reimbursement claims instead of cashless treatment.
Incorrect Information
Errors in claim forms or documents can slow down the process.
Frequently Asked Questions (FAQs)
What is a health insurance claim?
A health insurance claim is a request made to an insurance company for payment or reimbursement of medical expenses.
What are the two types of health insurance claims?
The two main types are cashless claims and reimbursement claims.
How long does the health insurance claim process take?
Processing times vary depending on the insurer, policy terms, and completeness of documents.
Can a health insurance claim be rejected?
Yes. Claims may be rejected if the treatment is not covered, documents are incomplete, or policy conditions are not met.
What documents are required for a health insurance claim?
Typical documents include:
-
Hospital bills
-
Medical reports
-
Discharge summary
-
Claim form
-
Prescriptions
What is cashless hospitalization?
Cashless hospitalization allows the insurance company to pay the hospital directly without the patient paying the full amount upfront.
Why is claim verification important?
Verification ensures that the claim meets policy conditions and prevents incorrect or fraudulent claims.
, benefits, and financial protection options available to policyholders. Many readers compare multiple guides before selecting a plan so they can clearly evaluate premiums, claim procedures, and long‑term advantages. A useful resource to explore is Cheap Health Insurance Options, which explains how this insurance policy works, the key benefits it offers, and situations where it may be the most suitable option. By reviewing this guide, you can gain deeper insights into coverage features, eligibility requirements, and practical tips that help individuals and families make smarter insurance decisions.
Conclusion
Understanding the health insurance claim process helps policyholders use their health insurance benefits effectively. When medical treatment is required, submitting a claim allows individuals to recover healthcare costs according to their policy coverage.
The claim process typically includes several key steps:
-
Receiving medical treatment
-
Notifying the insurer
-
Submitting necessary documents
-
Claim verification
-
Approval or rejection
-
Payment or reimbursement
Health insurance claims can be processed either through cashless claims, where the insurer pays the hospital directly, or reimbursement claims, where the patient pays first and later receives reimbursement.
Being familiar with the process helps reduce delays, avoid mistakes, and improve the chances of successful claim approval. By understanding policy terms, maintaining proper documentation, and following claim procedures carefully, policyholders can manage medical expenses more efficiently.
Disclaimer:
“Disclaimer: This article is for educational purposes only. Trust My Policy is an independent informational platform and does not sell insurance products or represent any insurance provider. Readers should consult official policy documents or licensed professionals for personalized advice.”